Prostatitis is an inflammation of the prostate, quite common today.
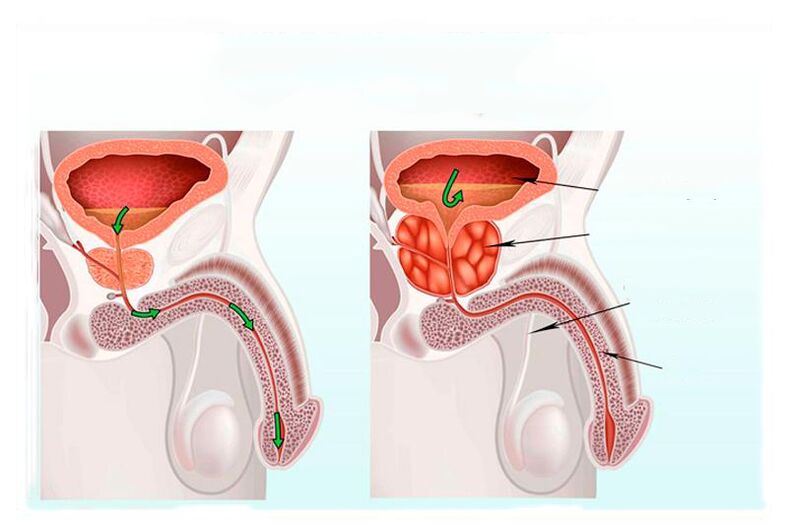
The prostate is a male organ and, therefore, the disease is also purely male.
Why is a prostate necessary? The prostate is responsible for the following functions:
- produces a liquid part of the sperm with the muscles of the bladder neck;
- produces an internal sphincter;
- turns testosterone into dihydrotestosterone.
The prostate or simply the prostate is located under the bladder, the urethra passes through the prostate and therefore the prostate is located around the urinary tube. And as the prostate enlarges during inflammation, it compresses the urinary tract and makes it difficult to urinate. Men over forty often suffer from prostatitis, this is a consequence of malfunction of the genitourinary system.
Factors that cause the development of prostatitis:
- hypothermia;
- infectious diseases;
- alcohol and tobacco use;
- trauma and hormonal disorders;
- sedentary work;
- urinary retention.
Prostatitis is divided into several types:
- Acute bacterial prostatitis: occurs during damage to prostate tissues with Escherichia coli, Pseudomonas aeruginosa, Staphylococcus aureus, etc.
- A large number of these bacteria are representative of a healthy microflora and live on our skin and stomach, but entering the tissues of the prostate, they cause inflammation. The main symptoms of acute bacterial prostatitis are nausea and pain in the groin and lower back, frequent trips to the bathroom and pain when urinating, intoxication of the body and decreased erection quality, signs of blood in the urine.
- Chronic bacterial prostatitis: occurs due to lesions of the genitourinary system or the presence of infections in organs.
- The symptoms of chronic prostatitis manifest as pain during urinary excretion and frequent fissure, discomfort in the groin, presence of blood in the semen, increase in body temperature by 0, 5-1 degree Celsius.
Chronic bacterial prostatitis occurs due to the lifting of heavy objects with a full bladder, as a result, urine enters the prostate, spasms of the pelvic muscles, therefore - increased pressure on the prostate, injury. The symptoms are also pain when urinating and only with laboratory tests can an infectious difference be detected.
Chronic prostatitis
Chronic prostatitis is a dangerous disease that, unlike prostatitis, carries with it a lot of unclear questions. What is chronic prostatitis? Chronic prostatitis is the presence of inflammation in the prostate, which is characterized by a series of tissue changes and functional disorders of the prostate, the activity of the male reproductive system. Chronic prostatitis is among the first diseases of the male reproductive system. The classification of chronic prostatitis is divided into several subspecies:
- acute bacterial prostatitis;
- chronic bacterial prostatitis;
- chronic abacterial prostatitis;
- inflammatory prostatitis with increased leukocytes in prostate secretions;
- noninflammatory process without increase in leukocytes;
- inflammation of the prostate without symptoms, which is randomly detected.
An infection caused by neurovegetative disorders causes and causes the development of chronic prostatitis. Hemodynamic disorders cause decreased immunity through autoimmune and biochemical processes. Factors in the development of chronic prostatitis are characteristics of the lifestyle that cause infection of the genitourinary system, frequent hypothermia and sedentary work, irregular sex life or the constant presence of a urethral catheter are also dangerous. Also important and dangerous agents that cause the disease will be disorders of the immune system, cytokines, bacteria of a low molecular weight polypeptide nature, which affect the functional activity of immune cells.
One of the main reasons for the development of non-inflammatory forms of chronic prostatitis is the dysfunction of the pelvic floor.
Symptoms of chronic prostatitis
Chronic prostatitis is pain and discomfort, dysfunction when urinating and sexual dysfunction. The presence of pain in the pelvic, perineum and groin region. Pain is often seen in the anus and scrotum. The sexual life is interrupted and the libido also decreases, but these signs are not observed in all patients. Chronic prostatitis is interchangeable in nature, the symptoms are aggravated and then muffled. In general, the symptoms of chronic prostatitis are similar to the stages of the inflammatory process. Pain in the scrotum and groin is characteristic of the exudative stage, as well as frequent urination, accelerated rash of semen and painful erections. The alternative stage is characterized by pain in the suprapubic part, normal urination and with accelerated semen eruption, pain during erections is not observed. In the proliferative stage, we can also see increased urination and the ejaculation process is slightly delayed. In the stage of prostate sclerosis, in addition to scar changes, the patient has pain in the suprapubic part, frequent urination and semen ejaculation is delayed or completely absent. It should also be borne in mind that the stages and disorders described above do not always appear and not for everyone.
To diagnose chronic prostatitis, as the disease is often asymptomatic, several tests and laboratory tests will help. The test is also important to help the doctor identify the intensity of symptoms, pain and urinary disorders. Laboratory testing for chronic prostatitis helps diagnose chronic prostatitis and possible prostate infection with atypical bacterial and fungal flora and viruses. If there is no bacterial growth in prostate secretions with an increase in the number of leukocytes, it is necessary to analyze whether there is chlamydia. Microscopic examination helps to reveal the number of leukocytes and mucus, Trichomonas and epithelium in the secretion of the urethra. The secret obtained after massage of the prostate is taken for bacteriological examination, and according to its results, the nature of the disease is determined. It is also important to conduct an immunological study, the results of which help to determine the stage of the disease and monitor the effect of treatment. The instrumental study of chronic prostatitis helps to determine the stage and form of the disease with additional observation throughout treatment. The ultrasound examination allows to study the size and volume of the prostate, the cyst structure and the sclerotic changes of the organ, the degree of expansion and the density of the contents of the seminal vesicles. Myography of the muscle and pelvic floor more information on suspected neurogenic urinary disorders. An X-ray study is performed to clarify the cause of the onset and course of further treatment for chronic prostatitis. Computed tomography of Organs pelvic organs is performed to exclude pathological changes in the spine and pelvic organs. Diagnosis as a way to exclude an illness unsuitable for symptoms helps to establish the nature of the pathological process: with inflamed processes in other organs; with diseases of the rectum; with sexual dysfunctions; with neuropsychiatric disorders, for example, depression or reflex sympathetic dystrophy.
Treatment of chronic prostatitis
The treatment of chronic prostatitis must be consistent and comprehensive. First, it is necessary to change the patient's habitual way of life and thinking. Also eliminate the influence of harmful factors, such as smoking and alcohol consumption, hypothermia. Thus, we interrupt the development of the disease and then bring about recovery. Even in the preparatory phase for treatment, adherence to the diet and the establishment of sexual life play an important role. The next main course in the treatment of the disease is the use of medications. This correct approach to the treatment of chronic prostatitis will help not only to fight the disease, but also to increase the effectiveness of treatment at all stages of the development of prostatitis. Chronic prostatitis does not usually require hospitalization, but in severe cases of chronic prostatitis, hospital treatment is more beneficial and more effective than outpatient treatment. Drug treatment leads to the establishment of good blood circulation in Organs pelvic organs, brings hormones and the immune system to normal levels. In such cases, antibacterial and immunomodulatory drugs, vasodilators and prostate massage are used. The use of antibacterial drugs is the basis for the treatment of chronic prostatitis. But, unfortunately, the effectiveness of this therapy has been proven, but not for all types of prostatitis. In chronic bacterial prostatitis, antibacterial treatment is effective; in chronic abacterial prostatitis, an empirical antibacterial treatment course is used.
At the moment, local physical treatment is very important. Physiotherapy with laser, mud and electrophoresis is considered the most effective. Electromagnetic radiation is based on anti-congestive and bacteriostatic action. Low-energy laser therapy stimulates microcirculation in the tissues of the prostate, and laser therapy also has a biostimulating effect. In the absence of contraindications, therapeutic prostate massages are used.
Surgical intervention is increasingly used in the treatment of prostatitis, as the disease affects more and more young men. An indication for surgery may be sclerosis of the seminal tubercle; these patients usually see a doctor with signs of lack of sexual sensation and ejaculation. In such cases, resection of the seminal tubercle is performed. In addition, surgery is used for sclerosis of the bladder and prostate.
Symptoms of prostatitis
Often, men who suffer from prostatitis complain of fever and increased body temperature, even if the temperature measured under the arm is normal, so, very often, the temperature in the anus will be high. Pain in the lower back, abdomen, perineum, anus and scrotum also serve as a signal to go to the doctor. Even more frequent urination, cramps and a burning sensation when urinating. There is a deterioration of the general condition, weakness, pain in the muscles and bones, severe headaches.
With inflammation of the prostate gland in men, it is difficult to urinate, which is usually accompanied by urinary retention. Constipation, which occurs due to compression of the rectum by an enlarged gland, is characteristic of the disease.
Treatment of prostatitis
Before starting treatment, you need to be sure of the exact diagnosis. The minimum manipulations that must be performed are measurement of the temperature in the anus, diagnosis and palpation of the lymph node inguinal perineum, general clinical examination of blood and general examination of urine. It will also be necessary to collect swabs from the urethra and bacterioscopy of urine and sediment. In addition, transrectal ultrasound of the prostate is performed.
In the anus, the temperature usually rises and differs from the temperature of the modes with the mouse by about one degree. In the analysis of urine, the leukocyte number indicator is exceeded. In blood tests, some changes are also highlighted, for example, the number of eosinophils decreases and neutrophilic leukocytosis appears. In immunosuppressed patients, sepsis is often seen with complications of prostatitis.
Upon palpation of the perineum, the patient feels pain, the patient has enlarged inguinal lymph nodes. The prostate is enlarged during palpation, swollen and hot to the touch, and sometimes with heterogeneous inflammatory seals. If the prostate is inflamed, the biopsy is not done and can spread the infection further.
The treatment of prostatitis consists of the use of antibiotics against the microorganisms that cause the disease. Antipyretics are also prescribed to lower body temperature and the use of emollient laxatives to facilitate bowel movements. The patient is prescribed a massage course, which consists of squeezing the inflamed secretion with your fingers, squeezing it in the ducts and, finally, in the urethra. Prostate massage improves blood circulation and has a good effect on prostate muscle tone.
Prevention of prostatitis
First, for the prevention of prostatitis, you should limit yourself to food and apply a special diet. You need to include foods like parsley, asparagus, strawberries in your diet, and if you like pasta and so on, they must be tough varieties. You must also exclude bad habits and alcohol, spicy foods. With an exacerbation of the disease, it is very important to exclude sex life.
For the prevention of prostatitis, it is necessary to exclude all risk factors for its occurrence, namely: observing adequate nutrition, excluding bad habits and having a regular sex life, since this does not allow the accumulation of sperm. Every boy should know that promiscuity in sexual intercourse is bad for the prostate. An active sex life increases the risk of contracting sexually transmitted diseases. Use contraceptives anyway. Monitor your intestines and go to the bathroom regularly. Another important point is work: if it is linked to physical inactivity, then you need physical activity, running will also help, swimming and tennis. Also, don't forget to take daily walks in the open air as they are very beneficial for the whole body. Hypothermia negatively affects the immune system and this is where the infection progresses. You must be examined by a urologist, even if there are no prerequisites for this.
Timely treatment of any urogenital infection will help to eliminate the cause of the development of prostatitis.
Folk remedies for the prevention of prostatitis are also popular, from them, there are recipes such as the inclusion of honey, nuts and dried fruits in the diet, which are rich in vitamins and minerals. Pumpkin and onion seeds, oats and seafood, liver and apples are rich in zinc and therefore have a special and important value and great benefits for the prostate. Add the tips above: empty your stomach completely and avoid constipation. This will help products like kefir, vegetable oil and vegetable fiber. Separately, it is necessary to mention the benefits of exercise for the inner muscles.
Prostatitis prevention exercises are easy and do not require special adaptations, they can be performed anytime and anywhere. Here are some examples of some of them: perform the movements of the perineum as if you were pulling the rectum; tense the muscles of the perineum, trying to stop urinating, keep them in this position as much as possible; while lying down, lift your pelvis and hold it for twenty or thirty seconds, repeat these movements until you feel pain and fatigue in your buttocks. These simple exercises will only be an advantage for your body.



























